Family-Focused Eye Care
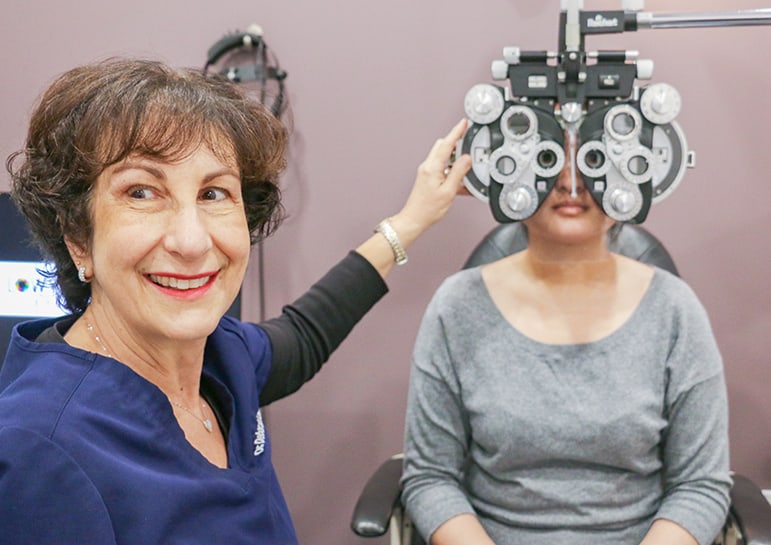
Our eye doctors at Lowy & Sewell Eye Care have proudly served the Thornhill community and surrounding area for over 30 years. We’ve seen generations of families come through our doors, and we value the relationships built through each visit. Our priority is providing comprehensive, compassionate care with every interaction—no matter how big or small.
We are a full service optometry practice offering annual eye exams, contact lenses, dry eye treatments, eye disease management & children’s care. Don’t forget to check out our extensive range of frames and lenses.
We look forward to seeing you soon.
Book Appointment

Personalized to You
Our team of eye doctors and eye care professionals are dedicated to helping our patients. Your vision and wellbeing are our top priorities, whether you need longer-lasting solutions for dry eye or help preventing your child’s growing nearsightedness. We strive to provide quality eye care personalized to support your vision and lifestyle.
Book AppointmentVisit Our Location
Lowy & Sewell Eye Care is located in the mall on the corner of Steeles Ave W and Dufferin St, on the west side, next to Max’s Restaurant. Free parking is available in the large lot steps from our front door.

Our Address
- 1520 Steeles Avenue W, Unit 119
- Concord, ON L4K 3B9
Contact Information
- Phone: 905-738-6680
- Email: [email protected]
Hours of Operation
- Monday: 9:00 AM – 6:00 PM
- Tuesday: 9:00 AM – 6:00 PM
- Wednesday: 9:00 AM – 7:00 PM
- Thursday: 9:00 AM – 6:00 PM
- Friday: 8:00 AM – 4:00 PM
- Saturday: 9:00 AM – 2:00 PM
- Sunday: Closed
Our Services
Our Brands
When it’s time to update your eyewear, stop by Lowy & Sewell Eye Care to browse our brands. Our friendly staff can help you find lenses customized to your daily needs and frames to bring a little fun and flair to your look.
We want to help your eyes look and feel their best. So whether you want to go bold or minimalistic—we have styles for you and your family.